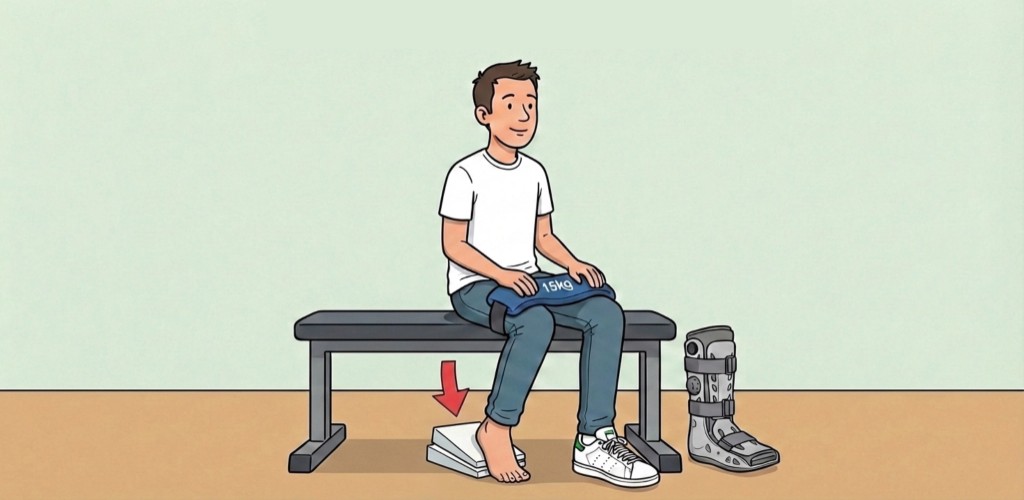
Seated calf raises after an Achilles tendon rupture are less about chasing a burn in the gym and more about reminding the healing tendon—gently—that it will bear load again in a pointed foot posture. Around week 6, many fracture and physio pathways allow the first guarded out-of-boot foot loading blocks: short sessions, tendon kept in plantarflexion (equinus — toes down relative to shin) often using a heel wedge, slant board, or instructions from your therapist—not casual barefoot stamping. Loads must climb slowly, pain-monitored, and inside the timetable that matches whether you had surgery vs non-operative care.
Contents
- Key takeaways
- What “week six” usually represents
- How seated raises differ from ordinary gym calf work
- Loads, wedges, and common progressions
- Evidence and protocol reality
- What this means for your recovery
- Frequently asked questions
- References
Key takeaways
- Early strengthening ≠ permission to stretch aggressively— protected plantarflexion loading preserves tendon approximation while tendon tissue is proliferating (see tendon healing primer](/blog/achilles-tendon-healing-early-protection)).
- Many teams aim for controlled, low-range calf contractions (seated calf raise with wedge) before transitioning to upright balance challenges—timing varies (elongation mechanics recap keeps the “why”).
- Load triad wins: exact angle, graduated weight, supervised dosing outperform copying random internet rep counts.
- Do not freestyle dorsiflexion, drop wedges early, jump to single-leg hopping, or ditch the boot prematurely—those mistakes drive elongation risk (re-rupture vs elongation).
- Signals like fresh pop, collapsing push-off confidence, escalating swelling, painless whole-leg swelling (clot vigilance/urgent pathways if taught) supersede incremental strength targets.
What “week six” usually represents
Week six lands inside the bridging phase where collagen callus gains organisation yet still behaves stretch-greedy if mis-loaded. Rehabilitation shifts from purely protective ambulation toward purposeful tendon tension—but still bounded.
Clinician variation is enormous:
| Typical pattern | Rough timing* | Aim |
|---|---|---|
| Solely boot gait + calf isometrics seated in brace | Weeks 2–8 | Controlled circulation, gait confidence |
| Seated wedge-biased plantarflexion raises supervised | Around weeks 4–8 commonly | Mild progressive tension without dorsiflexion overshoot |
| Standing double-leg calf holds with heel lift wedges | Criteria-based nearer boot wean | Eccentric lengthening postponed until safe |
*Your sheet supersedes any blog table.
Structured patient education—including recovery timeline FAQ and phased guides such as weeks 4–6—tracks these transitions when your clinic mirrors them.
How seated raises differ from ordinary gym calf work
| Feature | Everyday gym calf raise | Post-rupture protocol version |
|---|---|---|
| Ankle posture | Usually allows large dorsiflexion drop | Locks-in plantarflexion wedge bias |
| Load entry | Mirrors vanity strength goals | Criteria-based increments (~body weight pressure → handheld weight → thighs) |
| Volume | Chase fatigue | Respect tissue reaction—pain / fluid rules veto sets |
| Environment | Loud music optional | Therapist observation the first outings |
| End goal hypertrophy chase | Muscle burn | Preserve ideal tendon length mechanics (foot position recap) |
Standing raises, dorsiflexed drops, smith-machine nonsense come much later.
Loads, wedges, and common progressions
General pattern (adapt to your clinician’s script):
-
Setup: Foot forefoot on angled surface; heel free to drop minimally; torso tall; unloaded hands for balance—not levering dorsiflexion.
-
Activation: Gentle top-position squeeze (peak plantarflexion) for prescribed seconds or moderate reps—as directed.
-
Load ladders: Possibly sandbag/thigh weights analogous to illustrative 15 kg only if prescribed after tolerance checks—not because an infographic shows that mass.
-
Frequency: Typically little and often beats ego sets early.
-
Between sessions: Walking remains inside boot schedules until cleared; wedges inside boots advance only per wedge-removal pacing—not because the calf “feels ready.”
Night-time protection still matters (splint considerations) if dorsiflexion accidents happen historically.
Boot heel stacking interplay with wedges is unpacked in heel height fundamentals.
Evidence and protocol reality
Randomised Scandinavian non-operative “dynamic boot” care helped legitimise early protected motion alongside graded weight-bearing. In one blinded trial (Barfod and colleagues), patients in both arms followed a controlled early-motion dynamic protocol; the study contrasted immediate full weight-bearing versus six weeks non-weight-bearing. Achilles tendon scores at one year were similar, rerupture counts were low overall, and immediate weight-bearing modestly improved treatment-period quality of life—supporting the broad idea that protected loading can sit inside modern braced rehab, not permission to train unsupervised like a gym meme.
A later German assessor-blinded RCT compared early controlled ankle motion with immobilisation for non-operative care (British Journal of Sports Medicine, 2020). The exact exercises differ from wedge-biased seated raises, but both philosophies sit in the same family: start loading only with a written plan that limits dorsiflexion surprises (journal article page).
Evidence mapping functional progression (early protected motion and weight-bearing in boot-based protocols rather than prolonged cast-only care) derives from successive randomised cohorts(for example multicentre trials contrasting accelerated functional rehabilitation frameworks with older immobilisation-heavy approaches—Willits and colleagues, UK operative vs non-operative paradigm cohort).
Repair elongation physiology summaries (Diniz systematic review) justify angle neurosis: biomechanical fallout tracks imaging length shifts more cleanly than questionnaire noise—meaning disciplined plantarflexion loading is rational even when early motion trials differ in nuance.
Postoperative rehabilitation meta-analyses (for example Massen and colleagues summarising RCTs around operative repair rehab) emphasise supervised exercise dosage heterogeneity—another reason personal protocol documents beat blog generalisations.
No single trial mirrors every Instagram diagram; treat figures as teaching aids, not prescriptions.
What this means for your recovery
Do
- Photograph or print your exercise card so reps/loads stay honest.
- Log pain (0–10), next-day swelling, warmth—share trends with physio.
- Pair loading with sleep, protein adequacy—nutrition reality check—not magic stacks.
- Join structured education like our Achilles recovery course if you crave narrative pacing between appointments.
Don’t
- Hide symptoms to “keep streaks.”
- Symmetry-compete with the uninjured leg too early.
- Swap therapist wedge angles for spare books without sign-off.
Escalate urgently for pop, cannot trust push-off, new neurovascular red flags.
Frequently asked questions
Is week 6 mandatory for seated calf raises after an Achilles rupture?
No. Teams differ: some supervised loading starts nearer weeks 3–6, others keep most work inside the boot longer. Treat week six here as an idea—controlled calf loading begins when your protocol says it begins, guided by tenderness, wedge stage, operative vs non-operative pathway, and how you move day to day—not a meme calendar.
Why must the ankle stay pointed down during early seated raises?
Because pulling the toes up toward the shin (dorsiflexion) lengthens healing tendon fibres when collagen is still maturing—increasing tendon elongation risk. A wedge or slant keeps the toes plantarflexed so load pushes along the tendon in a clinician-approved angle. Different research programmes tighten or loosen allowable motion inside a brace—your job is disciplined execution of your rules, not debate-by-forum.
How much weight should I use?
Only what your clinician or physiotherapist prescribes—diagrams that show weights are teaching shorthand, not a universal dose. Typical progression travels from body-weight pressure → small handheld loads → weights on the thigh, audited in clinic before each jump.
Is mild discomfort normal?
Heavy work should not feel like a second rupture. Brief achiness or muscular fatigue can appear, but sharp tendon pain, new pop, rapid swelling, bruising tracking, breathlessness with calf pain, or painless whole-leg swelling are stop-and-escalate signals (use the urgent pathways your team gave; clot awareness matters in this window too).
When am I allowed dorsiflexion or stretching?
Timing is protocol-specific and often months after first seated loading. Aggressive calf stretching usually waits until the tendon is far more mature—many teams quote 12–18 months before hard end-range stretching goals in the same broad practice pattern we use elsewhere on this site. Until then, respect angle limits and build strength inside them.
References
-
Barfod KW, Bencke J, Lauridsen HB, Ban I, Ebskov L, Troelsen A. Nonoperative dynamic treatment of acute Achilles tendon rupture: The influence of early weight-bearing on clinical outcome: A blinded, randomized controlled trial. J Bone Joint Surg Am. 2014;96(18):1497-1503. DOI: 10.2106/JBJS.M.01273
-
Brumann M, Baumbach SF, Mutschler W, et al. Efficacy of early controlled motion of the ankle compared with immobilisation in non-operative treatment of patients with an acute Achilles tendon rupture: an assessor-blinded randomised controlled trial. Br J Sports Med. 2020;54(12):719-727. Article link
-
Willits K, Amendola A, Bryant D, et al. Operative versus nonoperative treatment of acute Achilles tendon ruptures: A multicenter randomized trial using accelerated functional rehabilitation. J Bone Joint Surg Am. 2010;92(17):2767-2775. DOI: 10.2106/JBJS.I.01401
-
Diniz LO, Pacheco J, Guerra-Pinto F, et al. Achilles tendon elongation after acute rupture: is it a problem? A systematic review. Knee Surg Sports Traumatol Arthrosc. 2020;28(12):4011-4030. DOI: 10.1007/s00167-020-06010-8
-
Massen FK, Shoap S, Vosseller JT, et al. Rehabilitation following operative treatment of acute Achilles tendon ruptures: a systematic review and meta-analysis. EFORT Open Rev. 2022;7(10):680-691. DOI: 10.1530/EOR-22-0072 (PMC free article)
Primary source: Barfod KW, Bencke J, Lauridsen HB, Ban I, Ebskov L, Troelsen A. Nonoperative dynamic treatment of acute achilles tendon rupture: the influence of early weight-bearing on clinical outcome