If you are wondering about blood clot risk after Achilles rupture, the short answer is yes: immobilisation in a boot increases risk, and your first week plan should include clot prevention. For most patients, that means a clear decision on blood thinners (daily injections or oral tablets), knowing the warning signs, and understanding exactly when to seek urgent help.
Rehabilitation still matters, but clot awareness is part of safe recovery, not an optional extra.
Contents
- Key Takeaways
- Why Clot Risk Rises After Achilles Rupture
- Routine vs Risk-Stratified Prophylaxis
- Injections vs Tablets: What Is the Difference?
- DVT and PE Red Flags: Your Action Plan
- What This Means for Your Recovery
- Frequently Asked Questions
- References
Key Takeaways
- Achilles rupture and boot immobilisation increase blood clot risk, especially early in recovery.
- Prophylaxis can be routine for many patients or risk-stratified using tools such as TRiP(cast).
- Common medication options are LMWH injections (for example enoxaparin) and oral tablets (for example rivaroxaban or apixaban).
- Learn the red flags now: new one-leg swelling, new calf pain, warmth, chest pain, breathlessness, or fainting.
- Sudden breathlessness or chest pain can mean a pulmonary embolism (clot in the lungs) and needs emergency care.
- Medication helps, but education and early reporting of symptoms are just as important.
Why Clot Risk Rises After Achilles Rupture
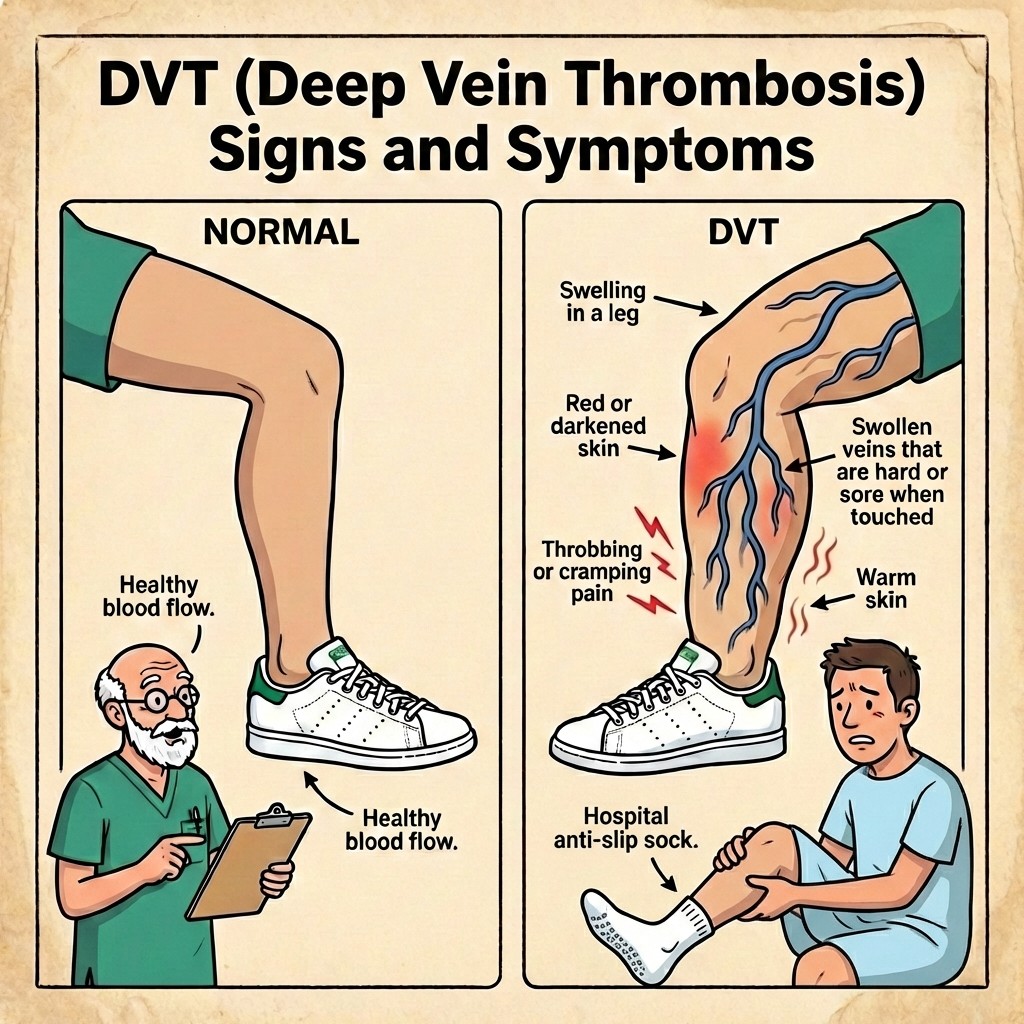
When your Achilles ruptures, your calf pump stops working normally because your ankle is immobilised. Blood flow in the deep veins slows down. At the same time, injury and inflammation increase clotting tendency. That combination raises risk of venous thromboembolism (VTE), which includes:
- DVT (deep vein thrombosis): clot in the leg vein
- PE (pulmonary embolism): clot that travels to the lungs (emergency)
If you want a broader primer on clot biology and symptoms, read our detailed guide: Blood Clot Risk After Achilles Rupture.
Routine vs Risk-Stratified Prophylaxis
Different services use different approaches:
| Approach | What it means | Pros | Limits |
|---|---|---|---|
| Routine prophylaxis | Most Achilles rupture patients receive blood thinners for a set period | Simple pathway, fewer missed high-risk patients | Some lower-risk patients may get treatment they do not need |
| Risk-stratified prophylaxis | Medication based on individual risk scoring (for example TRiP(cast)) | More personalised prescribing | Requires consistent assessment and documentation |
Recent implementation evidence for lower-limb immobilisation suggests many low-risk patients can safely avoid medication when assessed with a structured tool, while higher-risk patients should receive pharmacologic prophylaxis. In practice, your local protocol and clinician judgement still decide final treatment.
The key point for patients: ask your team which model they are using and why.
Injections vs Tablets: What Is the Difference?
If your team prescribes prophylaxis, the two most common options are injections and tablets.
| Option | Example | How taken | Typical practical issues |
|---|---|---|---|
| LMWH injection | Enoxaparin | Once-daily injection under the skin | Reliable and established, but daily self-injection can be hard |
| Oral anticoagulant tablet | Rivaroxaban or apixaban | Tablet by mouth | Easier to take, but not suitable for everyone |
Important notes:
- Tablets are often easier for adherence, but kidney function, bleeding risk, and drug interactions matter.
- Injection pathways are still widely used and may be preferred in some patients.
- Duration is commonly around the highest-risk immobilisation period, often about 4-6 weeks, but protocols vary.
If you are unsure why you were given one option and not the other, ask directly. A clear answer improves adherence.
DVT and PE Red Flags: Your Action Plan
DVT red flags (clot in the leg)
- New calf pain that feels different from your usual Achilles pain
- One-leg swelling that is increasing
- Warmth, redness, or unusual tightness in the calf
PE red flags (clot in the lungs) - emergency
- Sudden breathlessness
- Sharp chest pain
- Fainting or feeling close to collapse
- Coughing blood
| Symptom pattern | What to do |
|---|---|
| New suspicious leg symptoms only | Contact your fracture team or urgent care the same day for advice and likely ultrasound |
| Chest symptoms (with or without leg symptoms) | Call emergency services immediately |
Do not wait overnight to “see if it settles” when red flags are present.
What This Means for Your Recovery
- Confirm your clot plan before discharge. Ask whether your service uses routine or risk-based prophylaxis.
- Take medication exactly as prescribed. Missed doses reduce protection.
- Keep moving within protocol. Early protected loading supports circulation; see first 24-hour priorities.
- Do not ignore new symptoms. The fastest way to avoid serious complications is early review.
- Follow your own medical team if advice differs. Protocols vary between regions and individual risk profiles.
For boot setup and safe progression, also see Aircast vs VACOped and foot position after rupture.
Frequently Asked Questions
Do all Achilles rupture patients need blood thinners?
No. Some teams treat nearly everyone during immobilisation, while others use structured risk assessment and only treat higher-risk patients. Ask your team which approach they use for you.
Are tablets better than injections?
Not always. Tablets are usually easier to take, but injections can be the best choice depending on your bleeding risk, kidney function, and other medicines.
Can I still get a clot while on prophylaxis?
Yes. Risk goes down but does not become zero. You still need to watch for DVT and PE red flags.
Is calf pain always a clot after Achilles rupture?
No. Calf discomfort is common after rupture. The concern is new or changing pain, one-leg swelling, warmth, or tightness that does not fit your usual pattern.
What is the emergency symptom I should never ignore?
Sudden breathlessness or chest pain. Treat this as a possible pulmonary embolism and seek emergency help immediately.
References
- van Adrichem RA, Nemeth B, le Cessie S, et al. Targeted prophylactic anticoagulation based on the TRiP(cast) score in patients with lower limb immobilisation: a multicentre, stepped wedge, randomised implementation trial. Lancet. 2024;403(10431):1051-1060. DOI
- Samama CM, Laporte S, Rosencher N, et al. Rivaroxaban or Enoxaparin in Nonmajor Orthopedic Surgery. N Engl J Med. 2020;382:1916-1925. DOI
- Barfod KW, Nielsen EG, Olsen BH, et al. Risk of Deep Vein Thrombosis After Acute Achilles Tendon Rupture: A Secondary Analysis of a Randomized Controlled Trial. Orthop J Sports Med. 2020;8(4). PMC
- Nilsson-Helander K, Thurin A, Karlsson J, Eriksson BI. High incidence of deep venous thrombosis after Achilles tendon rupture: a prospective study. Knee Surg Sports Traumatol Arthrosc. 2009;17(10):1234-1238. PubMed
- Hashem M, Elbeshbeshy M, Khalafallah M, et al. Optimizing Venous Thromboembolism Prophylaxis in Achilles Tendon Rupture: A Systematic Review of Current Evidence and Protocol Recommendations. Cureus. 2025;17(10):e95184. PMC
Primary source: van Adrichem RA, Nemeth B, le Cessie S, et al.. Targeted prophylactic anticoagulation based on the TRiP(cast) score in patients with lower limb immobilisation