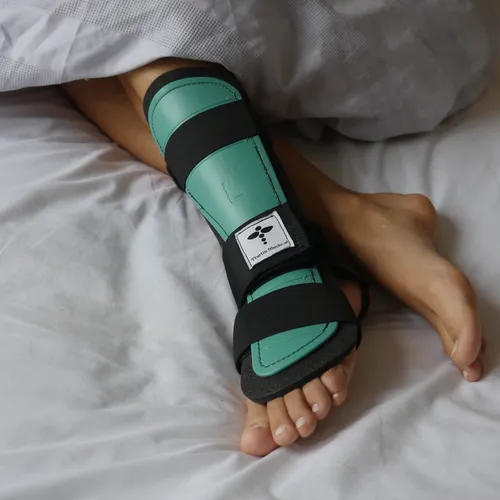
If you are searching for what to do in the first 24 hours after Achilles rupture, the answer is simple: protect the tendon first, progress later. In this early window, the main goal is not exercises, stretching, or testing movement. It is keeping the foot in a toes-down (plantarflexed) position, getting proper immobilisation, and avoiding anything that pulls the ankle upward.
That first day can shape how the tendon heals. Early protection helps reduce avoidable lengthening and gives you the best platform for strength later.
Contents
- Key Takeaways
- What Actually Happens at the Moment of Rupture
- The First 24 Hours: Protection Checklist
- Immobilisation and Weight-Bearing: What Patients Need to Hear Clearly
- Red Flags You Should Not Ignore
- What This Means for Your Recovery
- Frequently Asked Questions
- References
Key Takeaways
- The first day after rupture is about protection, not progress.
- Keep the ankle toes down in a boot, cast, or splint to help tendon-end approximation.
- Do not force dorsiflexion (toes up), stand barefoot, or remove support early.
- Ask for clear instructions on weight-bearing, crutch use, and follow-up timing before leaving emergency care.
- Learn red flags early: worsening calf swelling, chest symptoms, or a new pop should trigger urgent review.
- Brand matters less than protocol adherence: Aircast vs VACOped is secondary to correct setup and compliance.
What Actually Happens at the Moment of Rupture
Most patients describe the same story: a sudden snap, a feeling of being kicked in the heel, then immediate weakness. That shared experience is not exaggerated. When the Achilles ruptures, the normal tension across the tendon is lost.
In plain terms, the two torn ends need to be held in a position where the gap is not repeatedly stressed. Clinicians call this approximation. You are not trying to “heal it in one day.” You are trying to stop avoidable early setbacks while biology begins repair.
If you want a deeper explanation of why angle matters, see Foot Position After Achilles Rupture: Why Toes Down.
The First 24 Hours: Protection Checklist
Use this checklist as a practical script for the emergency phase:
| Priority | What to do now | Why it matters |
|---|---|---|
| 1. Immobilise immediately | Keep the ankle in a boot/cast/splint in plantarflexion | Helps maintain tendon-end approximation in the vulnerable early period |
| 2. Follow weight-bearing instructions | Walk only as advised, usually protected in the boot with aids if needed | Safe loading is protocol-based; unprotected loading is different |
| 3. Protect at all times | Do not stand or walk without protection | A single unprotected dorsiflexion event can stress fresh healing tissue |
| 4. Know the red flags | Ask exactly which symptoms require urgent return | Early detection of complications prevents bigger problems |
| 5. Arrange specialist follow-up | Confirm fracture clinic/foot-ankle review timing before discharge | Continuity of care reduces confusion and non-adherence |
Early clarity also reduces panic. Patients who know the plan are less likely to “test” the ankle or improvise.
Immobilisation and Weight-Bearing: What Patients Need to Hear Clearly
Good emergency care is not just putting on a boot. It is giving instructions the patient can actually use when they get home.
You should leave the first contact with answers to these questions:
- Can I weight bear now, and if so how much?
- Do I sleep in this boot or cast?
- When can I remove it, and for what?
- Who do I contact if symptoms change tonight?
Modern pathways often support early weight-bearing as tolerated in protection, which aligns with current clinical positions. But “early weight-bearing” never means barefoot walking or pushing the ankle into stretch. It means controlled loading inside the protection plan.
If your sleep setup is a problem, discuss options early. Night-time protection is a frequent weak point because unplanned ankle position in bed can stress the repair. For patients struggling with sleep positioning, a dedicated Achilles rupture splint can be part of a safer plan.
Red Flags You Should Not Ignore
The first 24 hours should include explicit safety advice, not generic reassurance.
Seek urgent medical review if you develop:
- Sudden chest pain, breathlessness, or coughing blood
- New, marked calf swelling or pain (especially one-sided and progressive)
- A new pop/snap with sudden loss of confidence in the leg
- Rapidly worsening pain, numbness, or colour change in the foot
Blood clot risk after Achilles rupture is real, which is why your team may discuss thromboprophylaxis and mobility strategy. We cover that in detail here: Achilles Rupture and Blood Clot Risk.
What This Means for Your Recovery
The first day sets your direction. It does not decide everything, but it can reduce avoidable mistakes.
Practical actions for patients and services:
- Use a standard discharge script for Achilles rupture (position, weight-bearing, red flags, follow-up).
- Treat angle progression like a prescription, not a comfort choice.
- Book early specialist review, not “see how it goes.”
- Give structured patient education in writing, not verbal advice alone.
- Start rehab at the right time, not immediately; see Achilles Tendon Healing: Why Early Protection Matters and the structured Achilles recovery course.
If advice differs between this article and your local hospital pathway, follow your treating team. Protocols vary between countries and clinicians.
Frequently Asked Questions
Should I start exercises in the first 24 hours?
Usually, no aggressive ankle exercises in the first day. The early priority is protection and positioning. Your team will introduce safe rehabilitation in stages.
Is it bad if I briefly moved my foot upward after the injury?
Not every brief movement causes harm. The concern is repeated or forceful unprotected dorsiflexion early on. Reset protection quickly and follow your plan.
Do I need surgery if I heard a loud snap?
Not necessarily. Current clinical positioning is that non-surgical care is first-line for many patients, with surgery reserved for specific indications. Early protection matters in both pathways.
Is one boot always better in the first day?
No single boot wins for everyone. Outcomes are usually driven more by fitting, positioning, and adherence than brand alone.
When should specialist follow-up happen?
As soon as practical after emergency presentation, typically through fracture clinic or foot-and-ankle service according to local protocol. Do not let follow-up become open-ended.
References
-
Collins R, Sudlow A, Loizou C, Loveday DT, Smith G. Closing the gap on Achilles tendon rupture: a cadaveric study quantifying the tendon apposition achieved with commonly used immobilisation practices. Foot Ankle Surg. 2018;24(2):124-127. PubMed
-
Qureshi SA, Ibrahim T, Rennie WJ, Furlong AJ. Dynamic Ultrasound Assessment of the Effects of Knee and Ankle Position on Achilles Tendon Apposition Following Acute Rupture. J Bone Joint Surg Am. 2011;93(24):2265-2270. PubMed
-
Aicale R, Tarantino D, Maffulli N. Management of Achilles and patellar tendinopathy: what we know, what we can do. J Foot Ankle Res. 2020;13:59. Context on tendon loading principles
-
Huttunen TT, Kannus P, Rolf C, Fellander-Tsai L, Mattila VM. Acute Achilles tendon ruptures: incidence and trends in surgery rates in Sweden between 2001 and 2012. Am J Sports Med. 2014;42(10):2419-2423. PubMed
-
Maffulli N, Oliva F, Costa V, Del Buono A. The management of acute and chronic Achilles tendon ruptures. J Orthop Surg Res. 2020;15:397. Open-access review
Primary source: Collins R, Sudlow A, Loizou C, Loveday DT, Smith G. Closing the gap on Achilles tendon rupture: a cadaveric study quantifying tendon apposition with commonly used immobilisation practices