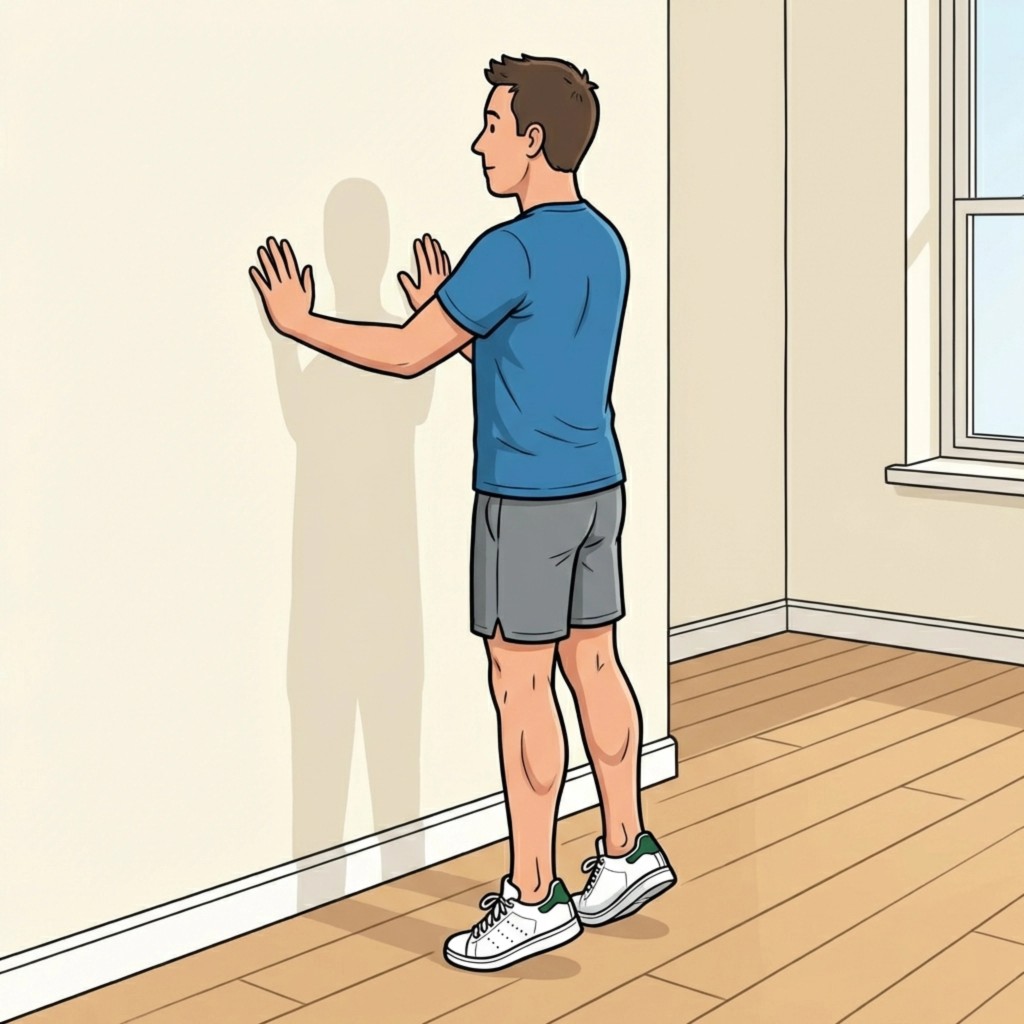
Standing calf raises after Achilles rupture are a key transition step. They move you from controlled, seated loading toward upright, weight-bearing strength—the position your tendon has to manage during walking.
But this is not a “just start standing” moment. The priority is load tolerance in a functional position: your tendon needs to handle the stiffness demands of bodyweight, while your balance and posture rebuild at the same time.
If you are currently doing seated calf raises, this post shows how and why you bridge to standing safely.
Contents
- Key takeaways
- Why standing is a bigger demand than seated work
- Seated vs standing: what changes (and why it matters)
- How to progress to standing calf raises
- What “good reps” look like
- When to progress beyond double-leg
- Why deficit raises come later
- What this means for your recovery
- Frequently asked questions
- References
Key takeaways
- Double-leg standing calf raises are a bridge exercise from seated strength to functional, weight-bearing loading.
- Progression should be criteria-based, guided by symptoms and movement quality—not only the calendar.
- Stability first: use a wall or support early to remove balance from the equation.
- No bounce: slow, controlled tempo keeps tendon loading predictable.
- Deficit/step variations generally come later because they add dorsiflexion demand and tendon strain.
Why standing is a bigger demand than seated work
When you do seated calf raises, you control:
- how much weight goes through the calf,
- how quickly you move,
- and how much your ankle is forced to move.
Standing work changes the game. Now the tendon has to cope with:
- bodyweight loading through an upright stance,
- more need for ankle alignment and postural control,
- and real-time adjustments to keep you stable.
That is why early standing calf raises are usually started as double-leg. Shared loading lets you rebuild tendon stiffness and control without overwhelming the recovering tissue.
For background on Stage 2 strength foundations, see seated calf raises and Stage 2 strength after boot removal.
Seated vs standing: what changes (and why it matters)
| Exercise | What it trains best | Main risk if progressed too fast |
|---|---|---|
| Seated calf raises | Force tolerance in a stable position | Overloading before your tendon is ready (symptom flare) |
| Double-leg standing calf raises | Reintroduces bodyweight load while keeping balance manageable | Compensated ankle control and a limp that sticks |
| Single-leg standing calf raises | One-limb tendon capacity and push-off readiness | Too much load on one side leading to gait asymmetry |
This is also consistent with broader Achilles rehab principles: weight-bearing and functional tasks are introduced progressively, but the tendon still has to tolerate the load, and movement quality matters.
How to progress to standing calf raises
If your clinician has cleared you to start standing calf raises, a common progression looks like this:
- Warm-up: 2–3 minutes of easy walking or gentle ankle movement (keep it light; no aggressive stretching).
- Use support: stand facing a wall or counter for balance.
- Start double-leg, flat ground: both feet on the floor.
- Keep it controlled: start with a small range and build toward full range only as you tolerate it.
- Increase load gradually: only after you can repeat sets with clean form.
Starting technique (double-leg, flat ground)
- Stand tall, knees straight or slightly soft (whatever keeps your ankle aligned).
- Rise through the whole foot and hold the top briefly if your clinician prefers (no shaking).
- Lower slowly—this is where you often feel the tendon do real work.
- Stop before form breaks.
For balance and coordination support during this transition, pair your calf work with Stage 2 balance and neuromuscular control.
What “good reps” look like
Use these quality checks:
- Heel height: can you reach a similar heel-rise height on the injured side (even if you start lower)?
- Smooth tempo: no sudden drops, no bouncing, and no jerking.
- Stable ankle alignment: avoid rolling out/in at the ankle.
- Symmetry of control: the movement should feel deliberate, not like the tendon is “catching.”
If you have trouble assessing quality, film a short clip from the side and behind. It makes compensation obvious and helps your physio adjust progression.
When to progress beyond double-leg
Once you can do double-leg standing calf raises with good control, the next step is usually:
- single-leg flat-ground heel raises on the way to functional performance.
When you are ready depends on how the tendon responds and how clean your reps are. A later milestone is covered in single-leg heel raise progression, including why some trainees should avoid “deficit” variations early.
As a practical rule:
- Don’t rush to harder variations if the basics look unstable.
- Progress control first, then load.
Why deficit raises come later
Deficit heel raises (off a step) increase dorsiflexion demand. In a recovering tendon, extra dorsiflexion and stretch exposure can raise elongation risk or simply provoke symptoms.
That is why most protocols prioritise:
- flat-ground standing loading,
- controlled range over maximal range,
- and load progression before stretch-heavy positioning.
If you are unsure whether your stage allows deficit work, ask your physiotherapist before trying it.
What this means for your recovery
Do:
- Start standing calf raises with double-leg and wall support until you have stable control.
- Use slow, controlled tempo and clean alignment.
- Track your next-day response (pain, stiffness, swelling) rather than judging only during the set.
Avoid:
- bouncing/momentum,
- skipping balance support too early,
- and adding steps/deficits before flat-ground control is consistent.
The objective is simple: restore strength in positions that reflect real-world demand—without exceeding tendon capacity.
Frequently asked questions
When should I start standing calf raises after Achilles rupture?
After you have a reliable seated foundation and your clinician clears you to progress to upright weight-bearing. This is generally criteria-based (symptoms and movement quality), not only time-based.
Why use double-leg standing calf raises first?
They share load between both legs and reduce balance demands, so you can reintroduce tendon stiffness work in a functional position more safely.
Should I bounce or use momentum?
No. Controlled tempo keeps tendon loading predictable and reduces uncontrolled stretch-heavy reps.
Can I do deficit (off-a-step) heel raises early?
Usually no. Deficit raises add dorsiflexion demand and tendon strain. Most protocols introduce higher-strain positions later once flat-ground control is stable.
What are signs I progressed too fast?
Increasing next-day pain, rising swelling, loss of heel-rise height, or a worsening limp usually mean you need to de-load and review progression with your physiotherapist.
References
-
Zellers JA, Carmont MR, Grävare Silbernagel K. Defining Components of Early Functional Rehabilitation for Acute Achilles Tendon Rupture: A Systematic Review. Orthop J Sports Med. 2019;7(11):2325967119884071. https://doi.org/10.1177/2325967119884071
-
Silbernagel KG, Steele R, Manal K. Deficits in Heel-Rise Height and Achilles Tendon Elongation Occur in Patients Recovering from an Achilles Tendon Rupture. Am J Sports Med. 2012;40(7):1568-1575. https://doi.org/10.1177/0363546512447926
-
Willits K, Amendola A, Bryant D, et al. Operative versus Nonoperative Treatment of Acute Achilles Tendon Ruptures: A Multicenter Randomized Trial Using Accelerated Functional Rehabilitation. J Bone Joint Surg Am. 2010;92(17):2767-2775. https://doi.org/10.2106/JBJS.I.01401
-
Silbernagel KG, Gustavsson A, Thomeé R, Karlsson J. A new measurement of heel-rise endurance with the ability to detect functional deficits in patients with Achilles tendon rupture. Knee Surg Sports Traumatol Arthrosc. 2010;18(2):258-264. https://doi.org/10.1007/s00167-009-0889-7
Primary source: Silbernagel KG, Steele R, Manal K. Deficits in Heel-Rise Height and Achilles Tendon Elongation Occur in Patients Recovering from an Achilles Tendon Rupture